
Laboratory Animal and Comparative Medicine ›› 2023, Vol. 43 ›› Issue (1): 3-10.DOI: 10.12300/j.issn.1674-5817.2022.089
• Animal Model of Human Disease: Pharmacology • Previous Articles Next Articles
Han LI1, Xiaorui ZHANG2, Chengfang ZHANG3( )(
)( )
)
Received:2022-06-20
Revised:2022-07-21
Online:2023-02-25
Published:2023-02-25
Contact:
Chengfang ZHANG
CLC Number:
Han LI,Xiaorui ZHANG,Chengfang ZHANG. Mechanism of Intermittent Fasting in Improving Olanzapine-induced Metabolic Disorders in Mice[J]. Laboratory Animal and Comparative Medicine, 2023, 43(1): 3-10. DOI: 10.12300/j.issn.1674-5817.2022.089.
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.slarc.org.cn/dwyx/EN/10.12300/j.issn.1674-5817.2022.089
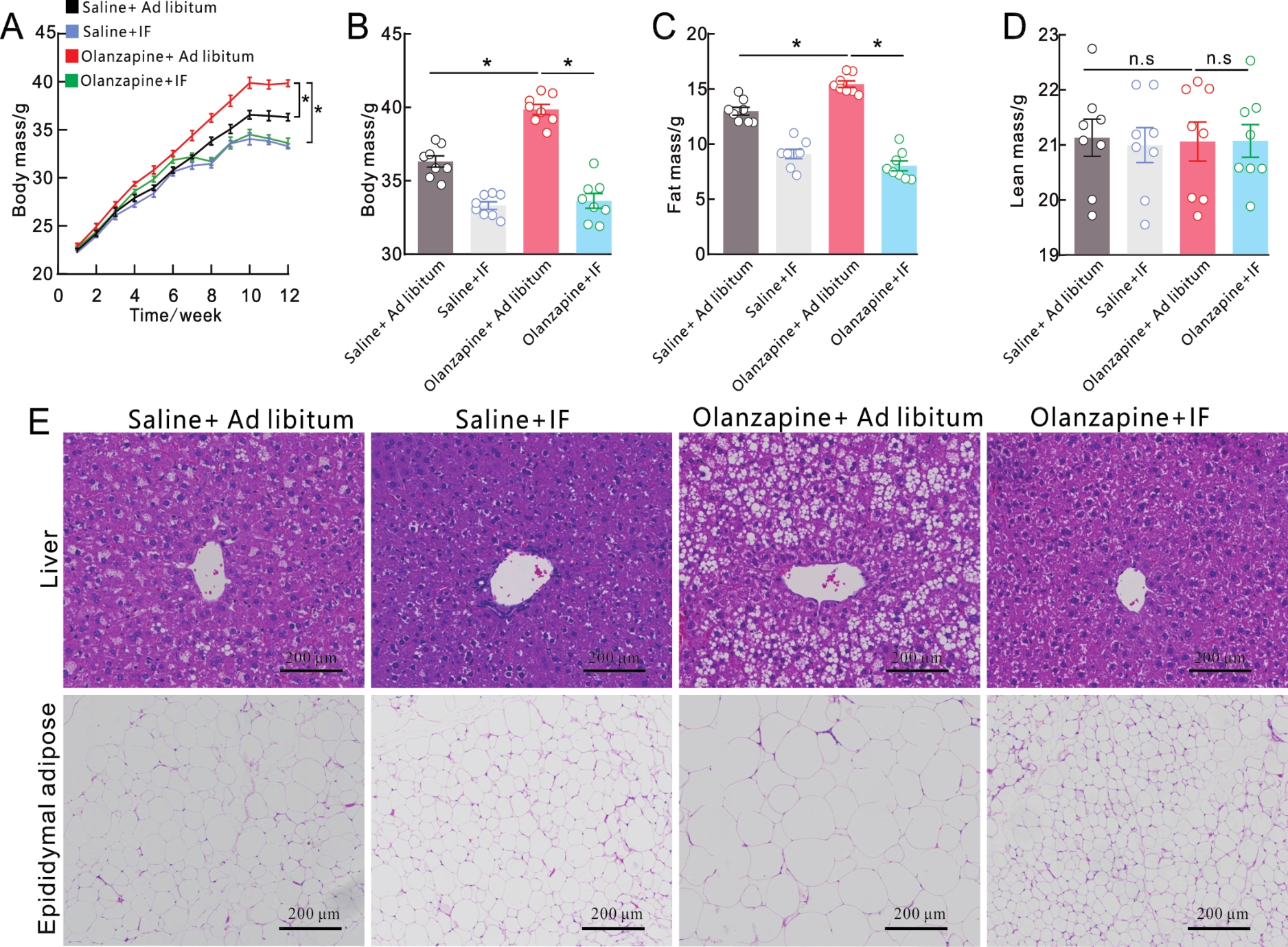
Figure 1 Effects of intermittent fasting on body mass, body fat distribution, visceral fat infiltration in olanzapine-induced miceNote:A, Body mass changes of mice in different treatment groups for 12 consecutive weeks (F=161.20, *P<0.001, two-way ANOVA followed by Turkey's post-test). B, Effect of intermittent fasting on body mass of mice with olanzapine diet for 12 weeks (*F=62.87,P<0.001, one-way ANOVA followed by Turkey's post-test). C, The changes of fat mass in mice after olanzapine diet for 12 weeks (*F=0.027,P<0.001, one-way ANOVA followed by Turkey's post-test). D, The changes of lean mass in mice after olanzapine diet for 12 weeks (n.sF=78.54, P=0.994,one-way ANOVA followed by Turkey's post-test). E, Liver and epididymal adipose morphology after olanzapine diet for 12 weeks(HE staining,the scale bar is 200 μm).
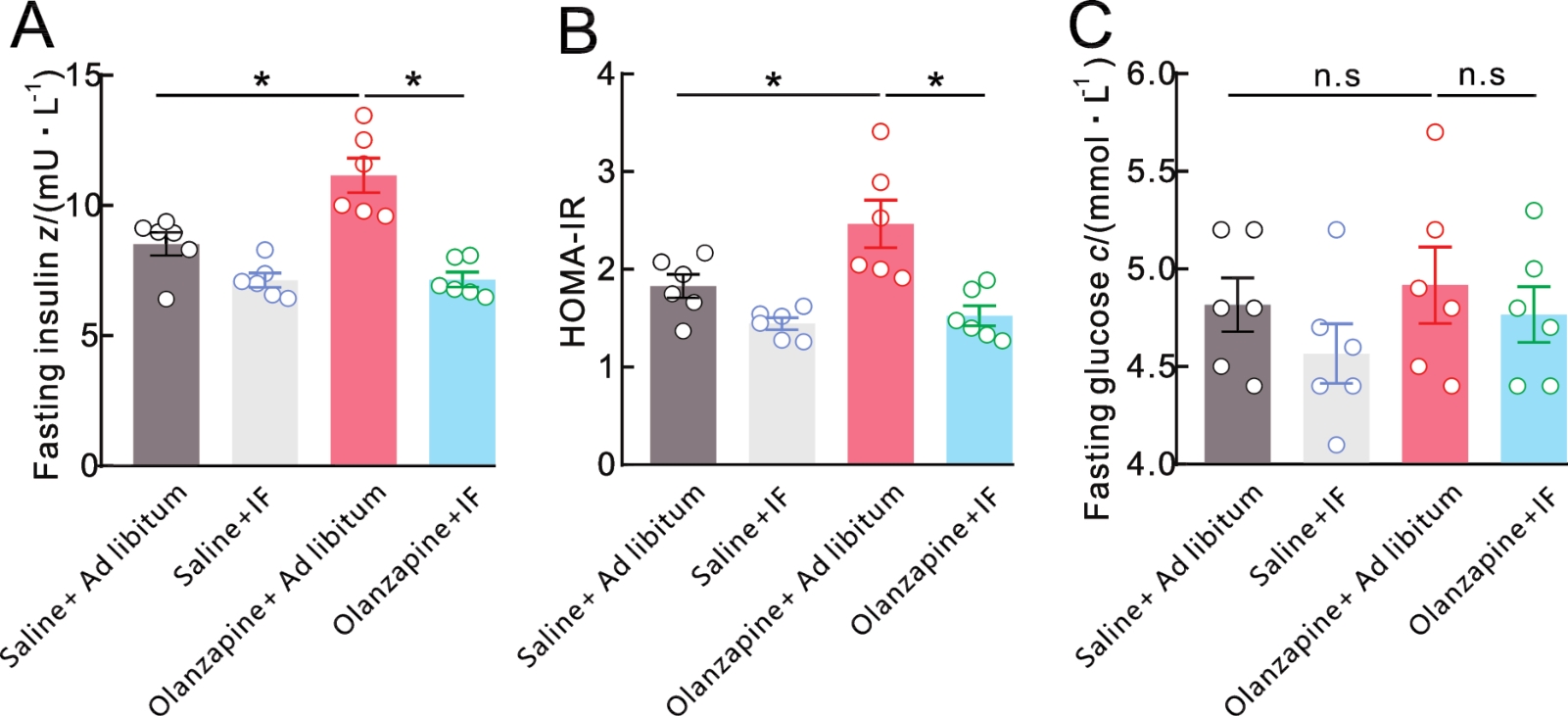
Figure 2 Effects of intermittent fasting on fasting blood glucose, insulin, and HOMA-IR, in olanzapine-induced miceNote:After 12 weeks of intermittent fasting, detecting fasting insulin levels (A) (*F=18.08,P<0.001, one-way ANOVA followed by Turkey's post-test), homeostatic model assessment of insulin resistance (HOMA-IR) (B) (*F=9.707, P=0.000 4, one-way ANOVA followed by Turkey's post-test), and fasting glucose levels (C) (n.sF=0.860, P=0.477, one-way ANOVA followed by Turkey's post-test).
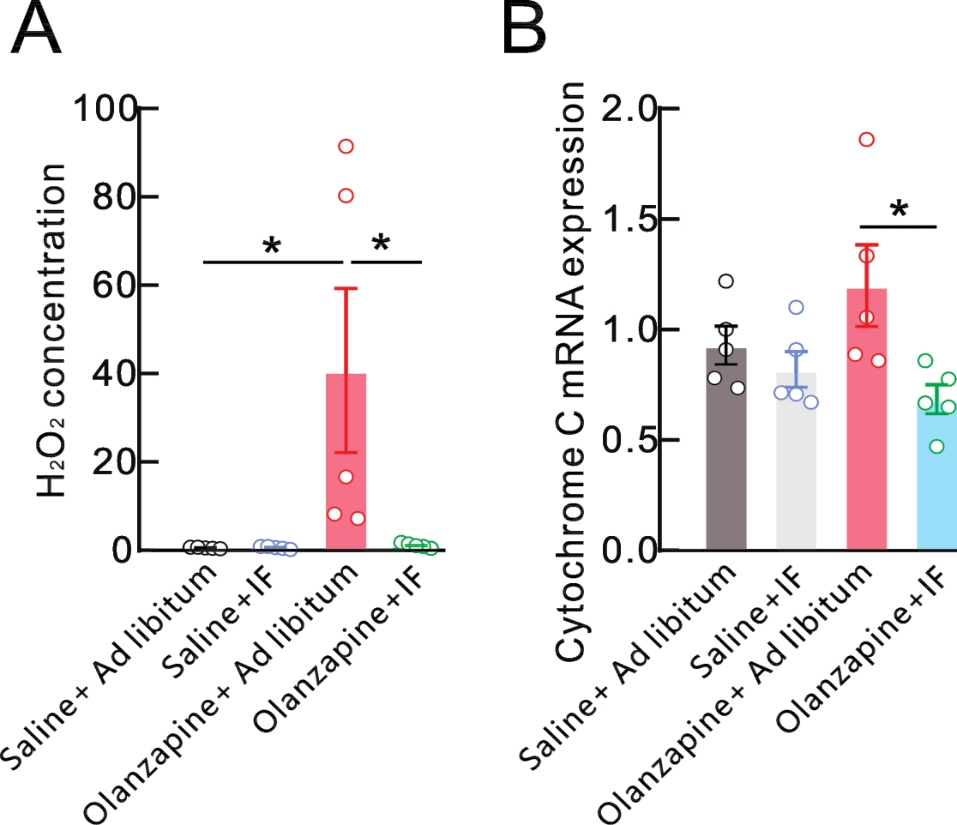
Figure 3 Effects of intermittent fasting on oxidative stress, mitochondrial function in olanzapine-induced miceNote:Hydrogen peroxide release was detected by ELISA (A)(*F=4.633, P=0.016), and the transcriptional level of Cytochrome C mRNA was detected by real-time fluorescence quantitative PCR (B)(*F=3.605, P=0.031) after 12 weeks of intermittent fasting treatment in mice.
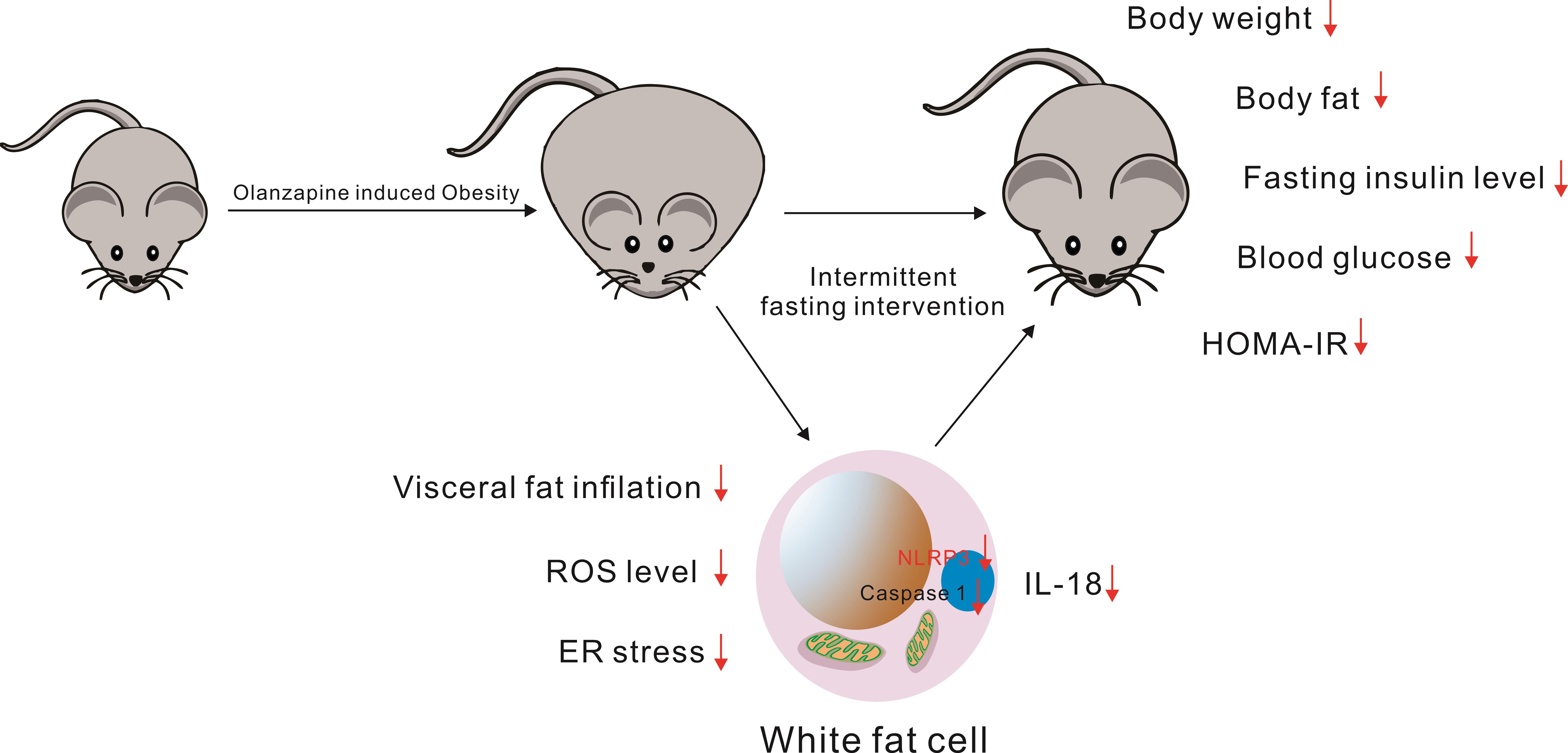
Figure 4 Schematic illustration of potential pathways underlying the mechanism of intermittent fasting in ameliorating olanzapine-induced metabolic disorders in mice
| 1 | STĘPNICKI P, KONDEJ M, KACZOR A A. Current concepts and treatments of schizophrenia[J]. Molecules, 2018, 23(8): E2087. DOI:10.3390/molecules23082087 . |
| 2 | JOHNSEN E, KROKEN R A, LØBERG E M, et al. Amisulpride, aripiprazole, and olanzapine in patients with schizophrenia- spectrum disorders (BeSt InTro): a pragmatic, rater-blind, semi-randomised trial[J]. Lancet Psychiatry, 2020, 7(11):945- 954. DOI:10.1016/S2215-0366(20)30341-2 . |
| 3 | CHENG Z, YUAN Y B, HAN X, et al. An open-label randomised comparison of aripiprazole, olanzapine and risperidone for the acute treatment of first-episode schizophrenia: eight- week outcomes[J]. J Psychopharmacol, 2019, 33(10):1227- 1236. DOI:10.1177/0269881119872193 . |
| 4 | POZNYAK A, GRECHKO A V, POGGIO P, et al. The diabetes mellitus-atherosclerosis connection: the role of lipid and lucose metabolism and chronic inflammation[J]. Int J Mol Sci, 2020, 21(5):1835. DOI:10.3390/ijms21051835 . |
| 5 | STANCU I C, CREMERS N, VANRUSSELT H, et al. Aggregated Tau activates NLRP3-ASC inflammasome exacerbating exogenously seeded and non-exogenously seeded Tau pathology in vivo[J]. Acta Neuropathol, 2019, 137(4):599-617. DOI:10.1007/s00401-018-01957-y . |
| 6 | BARRA N G, HENRIKSBO B D, ANHÊ F F, et al. The NLRP3 inflammasome regulates adipose tissue metabolism[J]. Bio chem J, 2020, 477(6):1089-1107. DOI:10.1042/BCJ20190472 . |
| 7 | MEYERS A K, ZHU X W. The NLRP3 inflammasome: metabolic regulation and contribution to inflammaging[J]. Cells, 2020, 9 (8):1808. DOI:10.3390/cells9081808 . |
| 8 | LIU Q Y, ZHANG D Y, HU D Y, et al. The role of mitochondria in NLRP3 inflammasome activation[J]. Mol Immunol, 2018, 103:115-124. DOI:10.1016/j.molimm.2018.09.010 . |
| 9 | MILLS E L, KELLY B, LOGAN A, et al. Succinate dehydrogenase supports metabolic repurposing of mitochondria to drive inflammatory macrophages[J]. Cell, 2016, 167(2):457-470.e13. DOI:10.1016/j.cell.2016.08.064 . |
| 10 | ANTONI R, JOHNSTON K L, COLLINS A L, et al. Effects of intermittent fasting on glucose and lipid metabolism[J]. Proc Nutr Soc, 2017, 76(3):361-368. DOI:10.1017/S002966511 6002986 . |
| 11 | LIANG B J, LIAO S R, HUANG W X, et al. Intermittent fasting therapy promotes insulin sensitivity by inhibiting NLRP3 in flammasome in rat model[J]. Ann Palliat Med, 2021, 10(5): 5299-5309. DOI:10.21037/apm-20-2410 . |
| 12 | HUANG Y Q, WANG Y, WANG H, et al. Prevalence of mental disorders in China: a cross-sectional epidemiological study [J]. Lancet Psychiatry, 2019, 6(3):211-224. DOI:10.1016/S2215- 0366(18)30511-X . |
| 13 | 徐若愚, 李献云. 精神分裂症认知行为治疗的研究进展[J]. 神经 疾病与精神卫生, 2022, 22(5):342-346. |
| XU R Y, LI X Y. Research progress of cognitive behavioral therapy for schizophrenic[J]. J Neurosci Ment Health, 2022, 22 (5):342-346. | |
| 14 | CARTERI R B, MENEGASSI L N, FELDMANN M, et al. Inter mittent fasting promotes anxiolytic-like effects unrelated to synaptic mitochondrial function and BDNF support[J]. Behav Brain Res, 2021, 404:113163. DOI:10.1016/j.bbr.2021.113163 . |
| 15 | MATTSON M P, LONGO V D, HARVIE M. Impact of intermit tent fasting on health and disease processes[J]. Ageing Res Rev, 2017, 39:46-58. DOI:10.1016/j.arr.2016.10.005 . |
| 16 | WU K K L, CHEUNG S W M, CHENG K K Y. NLRP3 inflammasome activation in adipose tissues and its implications on meta bolic diseases[J]. Int J Mol Sci, 2020, 21(11):4184. DOI:10.3390/ ijms21114184 . |
| 17 | ROTHMAN S M, GRIFFIOEN K J, WAN R Q, et al. |
| Brainderived neurotrophic factor as a regulator of systemic | |
| and brain energy metabolism and cardiovascular health[J]. | |
| N Y Acad Sci Ann, 2012, 1264(1):49-63. DOI:10.1111/j.1749-6632 . | |
| 2012.06525.x. | |
| 18 | LONGO V D, MATTSON M P. Fasting: molecular mechanisms and clinical applications[J]. Cell Metab, 2014, 19(2):181-192. DOI:10.1016/j.cmet.2013.12.008 . |
| 19 | ZHANG W J, CHEN S J, ZHOU S C, et al. Inflammasomes and fibrosis[J]. Front Immunol, 2021, 12:643149. DOI:10.3389/ fimmu.2021.643149 . |
| 20 | KAWAI T, AUTIERI M V, SCALIA R. Adipose tissue inflammation and metabolic dysfunction in obesity[J]. Am J Physiol Cell Physiol, 2021, 320(3): C375-C391. DOI:10.1152/ajpcell.00379.2020 . |
| [1] | WEI Yanye, SHEN Guo, ZHANG Pengfei, SHI Songping, HU Jiahao, ZHANG Xuzhe, HUA Huiyuan, HUA Guanyang, LU Hongzheng, ZENG Yong, JI Feng, WEI Zhumei. Dynamic Monitoring and Correlation Analysis of General Body Indicators, Blood Glucose, and Blood Lipid in Obese Cynomolgus Monkeys [J]. Laboratory Animal and Comparative Medicine, 2025, 45(1): 30-36. |
| [2] | Yisu ZHANG, Xinru LIU, Ruojie WU, Rui LIU, Hong OUYANG, Xiaohong LI. Establishment and Evaluation of Mouse Model of Pregnancy Pain-depression Comorbidity Induced by Chronic Unpredictable Stress, Complete Freund's Adjuvant and Formalin [J]. Laboratory Animal and Comparative Medicine, 2024, 44(3): 259-269. |
| [3] | Min LIANG, Yang GUO, Jinjin WANG, Mengyan ZHU, Jun CHI, Yanjuan CHEN, Chengji WANG, Zhilan YU, Ruling SHEN. Construction of Dmd Gene Mutant Mice and Phenotype Verification in Muscle and Immune Systems [J]. Laboratory Animal and Comparative Medicine, 2024, 44(1): 42-51. |
| [4] | Huiyan QIN, Huafeng CHEN, Hui YANG, Hailan LUO, Weizhong FU, Qingbo LI, Jiehong ZHANG. The Capacity of Silkworm Cocoon Water to Mitigate the Level of Oxidative Stress in Aged Rats [J]. Laboratory Animal and Comparative Medicine, 2022, 42(5): 393-400. |
| [5] | LI Zifa, ZHANG Hao, REN Meng, XU Kaiyong, HU Minghui, ZHOU Miaomiao, WANG Kezhou. Protective Effect of Quercetin on Lipid Metabolism Disorder in Mice Livers Caused by Cadmium [J]. Laboratory Animal and Comparative Medicine, 2021, 41(4): 305-312. |
| [6] | LI Hongbo, HUANG Rui, DAI Jiang, ZHONG Zhendong. Mechanism of Protective Effect of Raddeanin A on Hepatic Ischemia-reperfusion in Rats [J]. Laboratory Animal and Comparative Medicine, 2021, 41(1): 55-60. |
| [7] | LV Xiaojun, WU Sen, ZHANG Ju, XU Xiaoling, PAN Wangping, LI Hougang, WANG Pinghui, HE Kaiyong. Experimental Study on Establishment of Obesity Model in Rats Induced by High-Calorie Diet [J]. Laboratory Animal and Comparative Medicine, 2020, 40(5): 374-. |
| [8] | SHUI Yunhua, ZHANG Lan, LEI Guanglei, ZHU Yuanjiang, LI Peiyu. Effects of Ozonated Autohemotherapy on Melatonin and Oxidative Stress in Rats with Sleep Deprivation [J]. Laboratory Animal and Comparative Medicine, 2020, 40(2): 110-115. |
| [9] | LEI Shan, LIU Qiang, HUANG Wei-jin, WANG You-chun. Influence of Strain, Gender and Hair Coat of Mice on Establishing Bioluminescent Imaging Pseudovirus Mouse Model [J]. Laboratory Animal and Comparative Medicine, 2019, 39(6): 423-428. |
| [10] | Li Ying-niang, Dai Wei, Sheng Jian. Analysis of Goiter in Zebrafish [J]. Laboratory Animal and Comparative Medicine, 2019, 39(6): 462-466. |
| [11] | SHENG Yi-xuan, ZENG Guo-wei, YAO Liang-liang, LI Bing-tao, JIANG Li, ZHANG Qi-yun, XU Guo-liang. Observation on Correlation between Insulin Resistance Index and Blood Lipid in Obese Rats [J]. Laboratory Animal and Comparative Medicine, 2018, 38(6): 417-421. |
| [12] | PU Xiang-qiang, WANG Xiang, QIANG Guang-hui, MA Jin, DING Yue-yue, LV Hai-tao. The Dynamic Changes of Mitochondria in Endothelial Cells of Immunological Coronaritis in Mice [J]. Laboratory Animal and Comparative Medicine, 2018, 38(3): 169-175. |
| [13] | CHI Jun, GONG Hui, HE Yue-wei, WAN Ying-han, FEI Jian, KUANG Ying. Generation and Phenotyping Analysis of Lep Gene Knockout Mice [J]. Laboratory Animal and Comparative Medicine, 2017, 37(5): 344-351. |
| [14] | CHANG Kai, WANG Yu, PANG Wen-biao, GAO Ji-ping, CHEN Zhao-yang, SONG Guo-hua. Antagonistic Effect of Selenium on Change of Mitochondrial Membrane Potential of NRK-52E Cells Induced by Sodium Fluoride [J]. Laboratory Animal and Comparative Medicine, 2017, 37(3): 179-184. |
| [15] | YANG Hua, ZHAO Ya-Juan, OU Qiang. Establishment of Nonalcoholic Fatty Liver Fibrosis Model and Expression of Inflammatory Factors in Mice [J]. Laboratory Animal and Comparative Medicine, 2017, 37(1): 20-24. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||