
Laboratory Animal and Comparative Medicine ›› 2026, Vol. 46 ›› Issue (1): 46-54.DOI: 10.12300/j.issn.1674-5817.2025.044
• Animal Models of Human Diseases • Previous Articles Next Articles
LIU Chang1,2, XIANG Xuesong1, HE Huihuang1, CHEN Xiaoqing1, QIU Wenhong1( )(
)( )
)
Received:2025-03-20
Revised:2025-09-10
Online:2026-02-25
Published:2026-02-14
Contact:
QIU Wenhong
CLC Number:
LIU Chang,XIANG Xuesong,HE Huihuang,et al. Establishment and Evaluation of an Oxidative Stress Model of Atopic Dermatitis Induced by 2,4-dinitrofluorobenzene[J]. Laboratory Animal and Comparative Medicine, 2026, 46(1): 46-54. DOI: 10.12300/j.issn.1674-5817.2025.044.
Add to citation manager EndNote|Ris|BibTeX
URL: https://www.slarc.org.cn/dwyx/EN/10.12300/j.issn.1674-5817.2025.044
引物名称 Primer names | 引物序列 Sequences(5'→ 3') |
|---|---|
| RAGE-F | ACCGAGTCCGTGTCTACCGTAAG |
| RAGE-R | ATGAGGCCAGTGGAAGTCAGAGG |
| NLRP3-F | CGGTGGAGTGTCGGAGAAGAG |
| NLRP3-R | GATGCTGTCATTGTCCTGGTGTC |
| Caspase-1-F | GATGGCGATACACTCAGAGAACAC |
| Caspase-1-R | CAAGGAGGCAACTGGAGGAATG |
| IL-1β-F | CGAGGCACAAGGCACAACAG |
| IL-1β-R | ACAAAGAGGCAGAGAGACAGAGAG |
| GAPDH-F | AATTCCATGGCACCGTCAAG |
| GAPDH-R | AGCATCGCCCCACTTGATTT |
Table 1 Primer sequences for quantitative real-time PCR
引物名称 Primer names | 引物序列 Sequences(5'→ 3') |
|---|---|
| RAGE-F | ACCGAGTCCGTGTCTACCGTAAG |
| RAGE-R | ATGAGGCCAGTGGAAGTCAGAGG |
| NLRP3-F | CGGTGGAGTGTCGGAGAAGAG |
| NLRP3-R | GATGCTGTCATTGTCCTGGTGTC |
| Caspase-1-F | GATGGCGATACACTCAGAGAACAC |
| Caspase-1-R | CAAGGAGGCAACTGGAGGAATG |
| IL-1β-F | CGAGGCACAAGGCACAACAG |
| IL-1β-R | ACAAAGAGGCAGAGAGACAGAGAG |
| GAPDH-F | AATTCCATGGCACCGTCAAG |
| GAPDH-R | AGCATCGCCCCACTTGATTT |
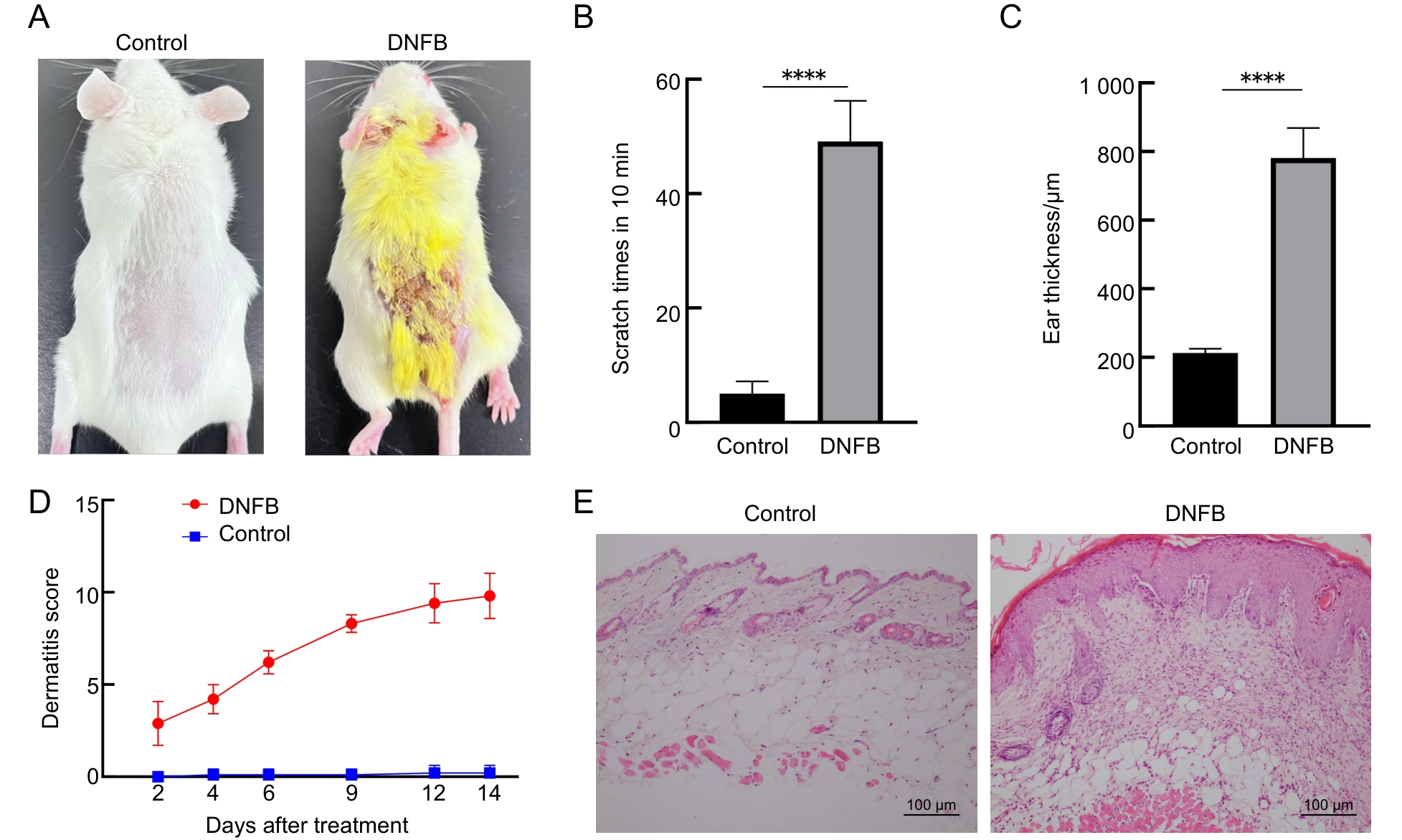
Figure 1 Assessment of skin inflammation and injury in a DNFB-induced mouse model of atopic dermatitis
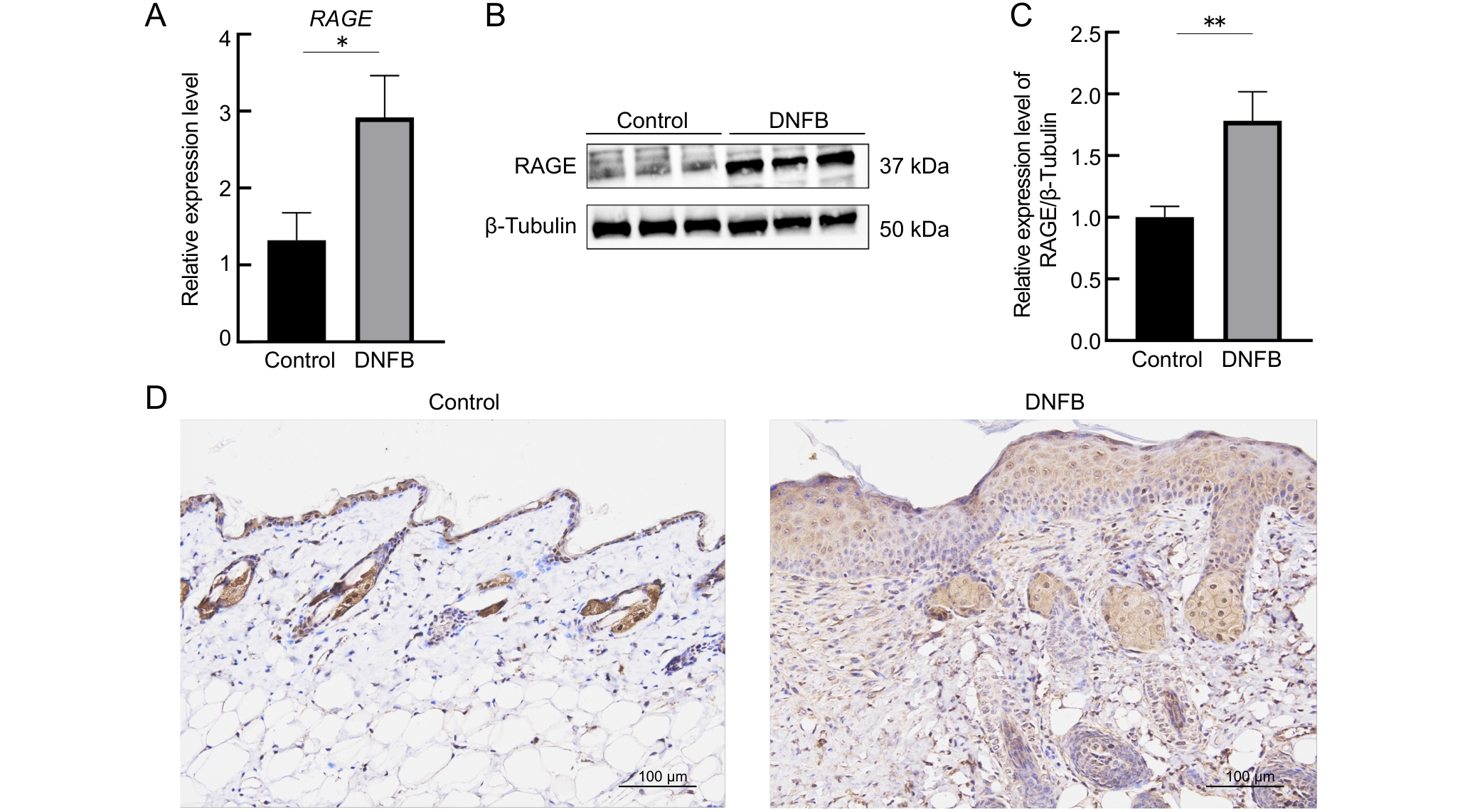
Figure 2 Changes in RAGE expression levels in skin tissues of mice in the DNFB-induced atopic dermatitis mouse model
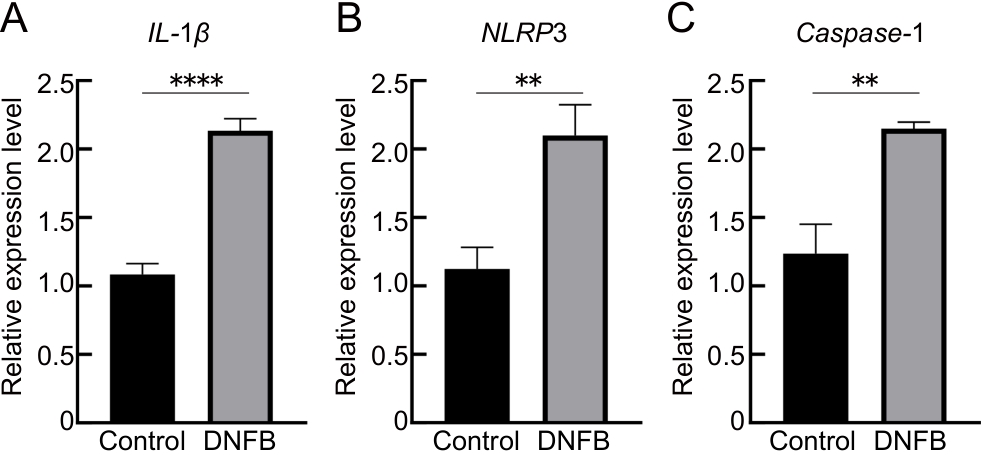
Figure 3 Changes in mRNA levels of IL-1β,NLRP3, and caspase-1 in skin tissues of atopic dermatitis mice induced by DNFB
| [1] | CHIRICOZZI A, MAURELLI M, CALABRESE L, et al. Overview of atopic dermatitis in different ethnic groups[J]. J Clin Med, 2023, 12(7):2701. DOI:10.3390/jcm12072701 . |
| [2] | BOOTHE W D, TARBOX J A, TARBOX M B. Atopic dermatitis: pathophysiology[M]//Management of Atopic Dermatitis: Methods and Challenges. Cham: Springer International Publishing, 2024: : 21-35. DOI:10.1007/978-3-031-54513-9_3 . |
| [3] | ITO T, NAKAMURA Y. The skin barrier and microbiome in infantile atopic dermatitis development: can skincare prevent onset?[J]. Int Immunol, 2024, 36(11):579-584. DOI:10.1093/intimm/dxae038 . |
| [4] | PUPPELS G J, HOURIHANE J O, NICO C, et al. Highly accurate, noninvasive early identification of infants with a filaggrin loss-of-function mutation by in vivo Raman spectroscopy, followed from birth to 12 months[J]. Ann Allergy Asthma Immunol, 2025, 134(4):457-464. DOI:10.1016/j.anai.2025.01.010 . |
| [5] | DEL DUCA E, HE H, LIU Y, et al. Intrapatient comparison of atopic dermatitis skin transcriptome shows differences between tape-strips and biopsies[J]. Allergy, 2024, 79(1):80-92. DOI:10.1111/all.15845 . |
| [6] | SAVVA M, PAPADOPOULOS N G, GREGORIOU S, et al. Recent advancements in the atopic dermatitis mechanism[J]. Front Biosci, 2024, 29(2):84. DOI:10.31083/j.fbl2902084 . |
| [7] | BANGERT C, ALKON N, CHENNAREDDY S, et al. Dupilumab-associated head and neck dermatitis shows a pronounced type 22 immune signature mediated by oligoclonally expanded T cells[J]. Nat Commun, 2024, 15(1):2839. DOI:10.1038/s41467-024-46540-0 . |
| [8] | WANG Z H, ZHANG H R, QI C H, et al. Ursolic acid ameliorates DNCB-induced atopic dermatitis-like symptoms in mice by regulating TLR4/NF-κB and Nrf2/HO-1 signaling pathways[J]. Int Immunopharmacol, 2023, 118:110079. DOI:10.1016/j.intimp.2023.110079 . |
| [9] | CHANG Q X, LYU J L, WU P Y, et al. Coffea arabica extract attenuates atopic dermatitis-like skin lesions by regulating NLRP3 inflammasome expression and skin barrier functions[J]. Int J Mol Sci, 2023, 24(15):12367. DOI:10.3390/ijms241512367 . |
| [10] | NIEHUES T, VON HARDENBERG S, VELLEUER E. Rapid identification of primary atopic disorders (PAD) by a clinical landmark-guided, upfront use of genomic sequencing[J]. Allergol Select, 2024, 8:304-323. DOI:10.5414/ALX02520E . |
| [11] | CHOI H, KIM S, KIM H J, et al. Sphingosylphosphorylcholine down-regulates filaggrin gene transcription through NOX5-based NADPH oxidase and cyclooxygenase-2 in human keratinocytes[J]. Biochem Pharmacol, 2010, 80(1):95-103. DOI:10.1016/j.bcp.2010.03.009 . |
| [12] | GAO J F, TANG L, LUO F, et al. Myricetin treatment has ameliorative effects in DNFB-induced atopic dermatitis mice under high-fat conditions[J]. Toxicol Sci, 2023, 191(2):308-320. DOI:10.1093/toxsci/kfac138 . |
| [13] | WANG Y, ZHANG Y, PENG G, et al. Glycyrrhizin ameliorates atopic dermatitis-like symptoms through inhibition of HMGB1[J]. Int Immunopharmacol, 2018, 60:9-17. DOI:10.1016/j.intimp.2018.04.029 . |
| [14] | ZHAO W, YU H H, MENG W W, et al. Icariin restrains NLRP3 inflammasome-mediated Th2 immune responses and ameliorates atopic dermatitis through modulating a novel lncRNA MALAT1/miR-124-3p axis[J]. Pharm Biol, 2023, 61(1):1249-1259. DOI:10.1080/13880209.2023.2244004 . |
| [15] | MU Z L, ZHAO Y, LIU X J, et al. Molecular biology of atopic dermatitis[J]. Clin Rev Allergy Immunol, 2014, 47(2):193-218. DOI:10.1007/s12016-014-8415-1 . |
| [16] | YIN T Y, FENG S, ZHU H, et al. Therapeutic potential of plasma-treated solutions in atopic dermatitis[J]. Free Radic Biol Med, 2024, 225:482-493. DOI:10.1016/j.freeradbiomed. 2024.10.290 . |
| [17] | MAJEWSKA-SZCZEPANIK M, ASKENASE P W, LOBO F M, et al. Epicutaneous immunization with ovalbumin and CpG induces TH1/TH17 cytokines, which regulate IgE and IgG2a production[J]. J Allergy Clin Immunol, 2016, 138(1):262-273.e6. DOI:10.1016/j.jaci.2015.11.018 . |
| [18] | XUE M L, LIN H Y, ZHAO R L, et al. Activated protein C protects against murine contact dermatitis by suppressing protease-activated receptor 2[J]. Int J Mol Sci, 2022, 23(1):516. DOI:10.3390/ijms23010516 . |
| [19] | ZHANG S, FANG X K, XU B L, et al. Comprehensive analysis of phenotypes and transcriptome characteristics reveal the best atopic dermatitis mouse model induced by MC903[J]. J Dermatol Sci, 2024, 114(3):104-114. DOI:10.1016/j.jdermsci. 2024.05.003 . |
| [20] | PÉNZES Z, HORVÁTH D, MOLNÁR P, et al. Anandamide modulation of monocyte-derived Langerhans cells: implications for immune homeostasis and skin inflammation[J]. Front Immunol, 2024, 15:1423776. DOI:10.3389/fimmu. 2024.1423776 . |
| [21] | KARACA O, AKARAS N, ŞIMŞEK H, et al. Therapeutic potential of rosmarinic acid in tramadol-induced hepatorenal toxicity: Modulation of oxidative stress, inflammation, RAGE/NLRP3, ER stress, apoptosis, and tissue functions parameters[J]. Food Chem Toxicol, 2025, 197:115275. DOI:10.1016/j.fct.2025.115275 . |
| [22] | SYED D N, ALJOHANI A, WASEEM D, et al. Ousting RAGE in melanoma: a viable therapeutic target?[J]. Semin Cancer Biol, 2018, 49:20-28. DOI:10.1016/j.semcancer.2017.10.008 . |
| [23] | DE OLIVEIRA I M, CHAVES M M. The NLRP3 Inflammasome in inflammatory diseases: Cellular dynamics and role in granuloma formation[J]. Cell Immunol, 2025, 411-412:104961. DOI:10.1016/j.cellimm.2025.104961 . |
| [24] | DE SIMONI E, CANDELORA M, BELLEGGIA S, et al. Role of antioxidants supplementation in the treatment of atopic dermatitis: a critical narrative review[J]. Front Nutr, 2024, 11:1393673. DOI:10.3389/fnut.2024.1393673 . |
| [25] | ZOU C C, LIU L, HUANG C Q, et al. Baiying qingmai formulation ameliorates thromboangiitis obliterans by inhibiting HMGB1/RAGE/NF-κB signaling pathways[J]. Front Pharmacol, 2022, 13:1018438. DOI:10.3389/fphar.2022.1018438 . |
| [26] | YU W Z, TAO M R, ZHAO Y L, et al. 4'-methoxyresveratrol alleviated AGE-induced inflammation via RAGE-mediated NF-κB and NLRP3 inflammasome pathway[J]. Molecules, 2018, 23(6):1447. DOI:10.3390/molecules23061447 . |
| [1] | Jianhua ZHENG, Yunzhi FA, Qiaoyan DONG, Yefeng QIU, Jingqing CHEN. Construction and Evaluation of a Mouse Model with Intestinal Injury by Acute Hypoxic Stress in Plateau [J]. Laboratory Animal and Comparative Medicine, 2024, 44(1): 31-41. |
| [2] | Han LI, Xiaorui ZHANG, Chengfang ZHANG. Mechanism of Intermittent Fasting in Improving Olanzapine-induced Metabolic Disorders in Mice [J]. Laboratory Animal and Comparative Medicine, 2023, 43(1): 3-10. |
| [3] | Huiyan QIN, Huafeng CHEN, Hui YANG, Hailan LUO, Weizhong FU, Qingbo LI, Jiehong ZHANG. The Capacity of Silkworm Cocoon Water to Mitigate the Level of Oxidative Stress in Aged Rats [J]. Laboratory Animal and Comparative Medicine, 2022, 42(5): 393-400. |
| [4] | LI Hongbo, HUANG Rui, DAI Jiang, ZHONG Zhendong. Mechanism of Protective Effect of Raddeanin A on Hepatic Ischemia-reperfusion in Rats [J]. Laboratory Animal and Comparative Medicine, 2021, 41(1): 55-60. |
| [5] | SHUI Yunhua, ZHANG Lan, LEI Guanglei, ZHU Yuanjiang, LI Peiyu. Effects of Ozonated Autohemotherapy on Melatonin and Oxidative Stress in Rats with Sleep Deprivation [J]. Laboratory Animal and Comparative Medicine, 2020, 40(2): 110-115. |
| [6] | JIA Huan-huan, ZENG Ye-wen, LUO Ting, GONG Bao-yong, MAI Dong-mei, PAN Ying-chun, ZHAO Wei-bo. Effects of Different Concentrations of Chromium-containing Bedding Materials on Toxity of Blood and Organs in BALB/c Nude Mice and KM Mice [J]. Laboratory Animal and Comparative Medicine, 2019, 39(6): 454-461. |
| [7] | JI Lian, MA Tie, DI Zheng-hong, Liu Dong-yan. Establishment of Atopic Dermatitis Mouse Model [J]. Laboratory Animal and Comparative Medicine, 2018, 38(4): 267-271. |
| [8] | WANG Hong, WEI Jie, LI Xiao-bo, GONG Wei, YUE Bing-fei. Application of Biochemical Markers on Analysis of Population Genetic Structure in KM mice [J]. Laboratory Animal and Comparative Medicine, 2017, 37(2): 144-149. |
| [9] | LIU Xue-xu, YANG Wen, DING Yun-ping. Mouse Model for Fetal Growth Restriction in Pregnant Metaphase by Limited Feeding [J]. Laboratory Animal and Comparative Medicine, 2015, 35(6): 453-457. |
| [10] | ZENG Xian-cheng, MA Jing, CHANG Yan, LIU Quan-hai. Progress on Monitoring Methods of Oxidative Stress after Stress in Laboratory Animals [J]. Laboratory Animal and Comparative Medicine, 2012, 32(6): 549-552. |
| [11] | XU Xiao-ping, PAN Yong-ming, CHEN Liang, XU Jian-qin, WANG De-jun, ZHU Ke-yan, YANG Yu-wei, CHEN Min-li. Observation on Oxidative Stress in Chronic Myocardial Ischemia in Mini-pig [J]. Laboratory Animal and Comparative Medicine, 2012, 32(5): 401-406. |
| [12] | LU Xiao-cong1,LIN Qiao2, WANG Yu-E2,WANG You-Wei1. Changes of Immune Function in Closed Colony of KM Mice after Biocleaning [J]. Laboratory Animal and Comparative Medicine, 2004, 24(1): 23-25. |
| [13] | SHI Mei-lian1,ZHU Dong-qin2, GU Jian-zhong2, LIU Li-jun1,BAO Shi-min1 MAO Jia-xian2, SHI En1, ZHANG Rui-zhong2, CHEN Guo-qiang2 MAO Jia-xian2, ZHAO Guo-ji1, FU Jie2,XIE En2, XU Ping1. Measurement for Organ Weight of KM Mice from 6 Colonies in China [J]. Laboratory Animal and Comparative Medicine, 2001, 21(3): 143-146. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||